|
8/17/2023 0 Comments Distal tibia fibula fracture
The locking screws were inserted only and only when the fracture reduction was satisfactory. Non locking screws were inserted first in either the proximal or distal fragment as required to aid in the reduction of the fracture so as to pull the bone to the plate. Following confirmation, a drill bit or K-wire was used to fix the plate onto the tibia. The plate was centred on the proximal fracture fragment in both antero-posterior and lateral views with the help of a locking sleeve inserted into the most proximal hole. The thumb was kept anteriorly on the tibial crest and was used to guide the proximal part of the plate onto the antero-medial surface of the tibia. Smooth and gentle supination-pronation motions were used while inserting the plate. 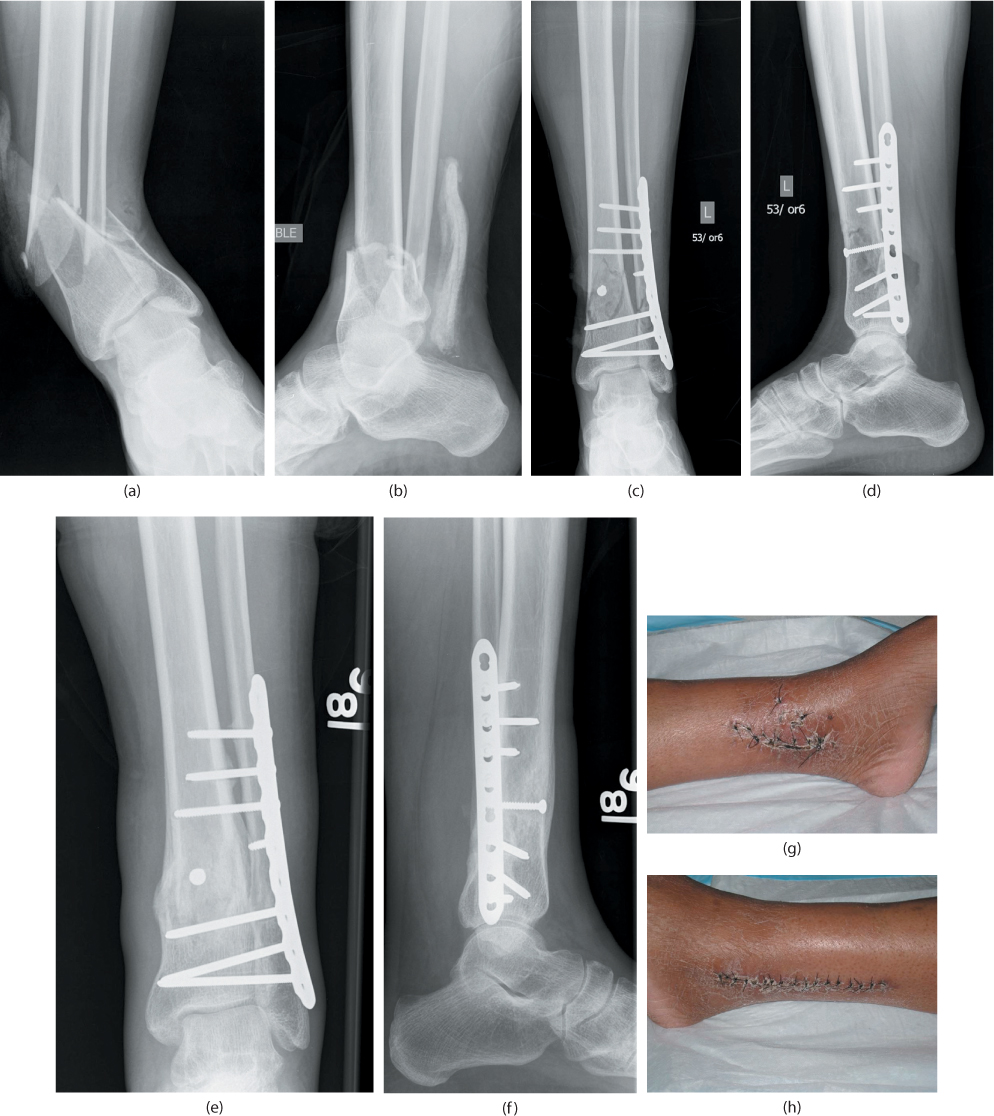
The plate was tunnelled proximally subcutaneously across the fracture site, using the locking sleeve as the handle with a dagger hold. Then the selected locking compression plate with a locking sleeve screwed into its distal hole was held with a pen-like grip. If the associated fracture fibula required fixation, it, was fixed by rush nail or one third tubular plate according to the fracture type, before fixation of the tibia.Īfter provisional reduction, a 3–4 cm vertical incision was given at the centre of the medial malleolus and a subcutaneous tunnel was opened with a haemostat or artery forceps. The mechanical axis and anatomical axis of the lower limb was checked with the cautery cord. Angulation, length of tibia and fibula, rotation and integrity of the ankle mortise were considered. The reduction was assessed repeatedly using visual and fluoroscopic control.  
In severely comminuted fractures, a femoral distractor was used. The type and likely length of the plate was calculated. The fibular fracture was noted and surgical plan decided accordingly. X-rays taken were evaluated for fracture morphology, level and extent of comminution. Patients with precarious skin condition were managed with limb elevation, regular dressing care and prophylactic intravenous antibiotics surgery was delayed till appearance of the ‘wrinkle sign’, but performed within 2 weeks from trauma. The leg was immobilised in a plaster slab till definitive surgery. Standard antero-posterior and lateral radiographs of the affected leg with knee and ankle joint were taken. We excluded patients with pathological fractures, fractures older than 2 weeks, Gustilo and Anderson Type II and Type III fractures, and patients who were unfit for surgery.Īfter stabilising the traumatised patient, routine pre-anaesthetic investigations were carried out. Informed consent for both the surgery and inclusion in the study were taken before the procedure. All closed fractures and Gustilo and Anderson Grade I compound fractures of the distal third tibia, with or without intra articular extension, upto 2 weeks old were included in the study. The study was approved by our institutional ethics committee and written informed consent was obtained from all patients. A total of 50 patients with a mean age of 36 years were included. 11,12 We reviewed the clinical indications and efficacy of MIPO in distal third tibia.įrom May 2010 to May 2013, we conducted a prospective case series at our Level 1 trauma centre. Minimally invasive submuscular and subcutaneous plate fixation (MIPO) can address several of the issues associated with intramedullary nailing, while amalgamating all biological benefits of closed reduction and fixation. The recent innovation of nails with tip locking is a testimony that earlier nails were insufficient fixation tools for distal tibia however tip locking is technically difficult and fractures that require it are essentially difficult to fix with nails. 8 Concerns regarding difficulties with reduction/loss of reduction, inappropriate fixation in fractures with articular extension, anterior knee pain 9 and hardware failure have slowed the acceptance of intramedullary nailing as a treatment of fractures of the distal tibia. 6,7 However, proximal and distal shaft fractures can be difficult to control with an intramedullary device, increasing the frequency of malalignment. The intramedullary nail spares the extraosseous blood supply, allows load sharing, and avoids extensive soft tissue dissection. In current orthopaedic practice, minimally invasive plating osteosynthesis (MIPO) and interlocking nailing are the preferred techniques for fractures of the distal third tibia. Small wire fixators, 1–3 and Open reduction and plating, 4,5 have been used with varying results. These fractures can be managed with various techniques. Fractures of the distal third tibia are unique in that the bone is subcutaneous with depleted muscular cover the consequent decreased vascularity leads to complications like delayed bone union, wound complications such as dehiscence and infection.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
